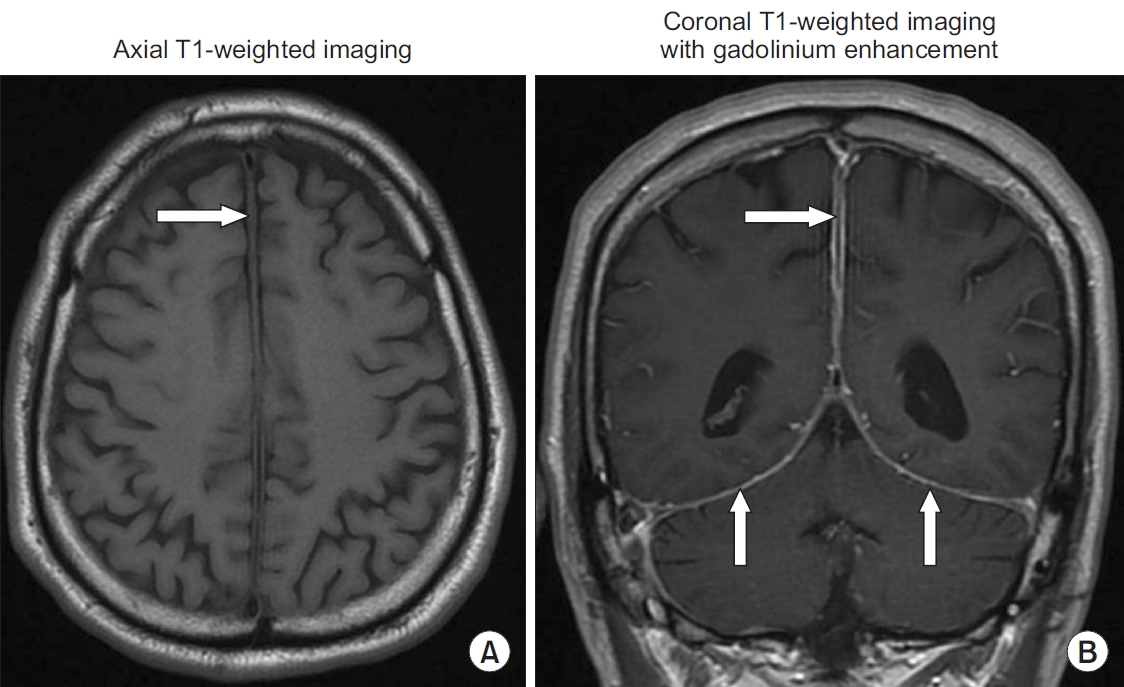
A 66-year-old man presented with fever and headache that had lasted for 3 months. The headache had a continuous pressing quality and bilateral involvement. He had a history of undifferentiated arthritis, for which he had undergone a treatment with chroloquine, leading to disease remission 2 years prior. He also had long term hypertension and diabetes. Current medications included enalapril, metformin, and chroloquine. He was febrile with body temperature of 38.5┬░C. Neither nuchal rigidity nor lymphadenopathy was detected. The findings of other general and neurological examinations were unremarkable. Magnetic resonance imaging (MRI) of the brain revealed thickening of the falx cerebri with diffuse pachymeningeal enhancement (
Figure 1). A lumbar puncture revealed an opening pressure of 200 mm H
2O. Cerebrospinal fluid (CSF) analysis showed a white blood cell count of 785 cells/mm
3 with 62% lymphocytes and 38% neutrophils, a protein level of 72 mg/dL, and a glucose level of 80 mg/dL (concurrent a blood glucose level of 182 mg/dL). The results of Gram and Ziehl-Neelsen staining, India ink preparation, cryptococcal antigen, tuberculosis polymerase chain reaction, and culture for bacteria were negative. The CSF culture, which was subsequently reported, was also negative for
Mycobacterium tuberculosis . The adenosine deaminase (ADA) level in CSF, which was determined by an automated method, was 11.1 U/L. Blood serological study for Venereal Disease Research Laboratory was nonreactive. The result of a chest X-ray was within the normal limits. The patient denied performing the meningeal biopsy. Diffuse hypertrophic pachymeningeal tuberculosis was suspected due to the patient having symptoms of prolonged fever and headache, lymphocytic CSF pleocytosis with elevated protein level and low CSF-to-serum glucose ratio, and a high level of CSF-ADA. The patient was treated with combined antituberculous drugs [isoniazid (I), rifampin (R), pyrazinamide (Z), ethambutol (E)], for 2 months, followed by IR (isoniazid, rifampin) for 4 months [
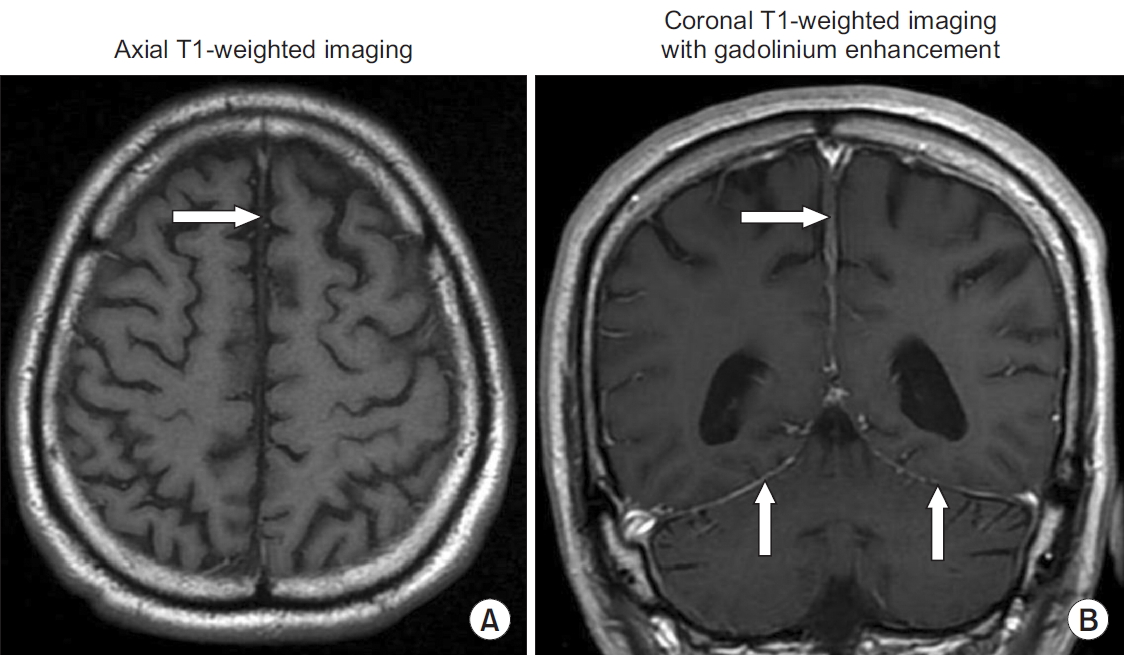
1]. The fever and headache gradually disappeared. A follow-up MRI of the brain revealed a marked decreased in the thickening of the falx cerebri and pachymeningeal enhancement (
Figure 2). The results of repeat CSF analysis and the level of CSF-ADA were within normal ranges.
Hypertrophic pachymenigitis is a rare disease and consists of localized or diffuse thickening of the dura mater. It can involve the cranial or the spinal dura or both. Neurological manifestations include chronic headache, cranial nerve palsies, and progressive other neurological deficits arising due to compression of neural structures by the enlarged dura mater. The etiologies of this disorder divide into primary (idiopathic) and secondary causes; including infections (tuberculosis, fungal infection, cysticercosis, syphilis), systemic disorders, and malignancies [
2]. Initial diagnosis depends on radiological findings which reveals focal or diffuse thickening of the dura. Dural tuberculosis is rare and usually presents with localized involvement of the pachymeninges [
3]. In this patient, the diagnosis of pachymeningeal tuberculosis was confirmed by clinical response to antituberculous treatment [
4].
This report also demonstrates the clinical utility of CSF-ADA as a one of diagnostic tests in the diagnosis of central nervous system tuberculosis [
5].







 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Print
Print Download Citation
Download Citation



