Nonspecific Bronchoprovocation Test
Article information
Abstract
Bronchial asthma is a disease characterized by the condition of airway hyper-responsiveness, which serves to produce narrowing of the airway secondary to airway inflammation and/or various spasm-inducing stimulus. Nonspecific bronchoprovocation testing is an important method implemented for the purpose of diagnosing asthma; this test measures the actual degree of airway hyper-responsiveness and utilizes direct and indirect bronchoprovocation testing. Direct bronchoprovocation testing using methacholine or histamine may have superior sensitivity as these substances directly stimulate the airway smooth muscle cells. On the other hand, this method also engenders the specific disadvantage of relatively low specificity. Indirect bronchoprovocation testing using mannitol, exercise, hypertonic saline, adenosine and hyperventilation serves to produce reactions in the airway smooth muscle cells by liberating mediators with stimulation of airway inflammatory cells. Therefore, this method has the advantage of high specificity and also demonstrates relatively low sensitivity. Direct and indirect testing both call for very precise descriptions of very specific measurement conditions. In addition, it has become evident that challenge testing utilizing each of the various bronchoconstrictor stimuli requires distinct and specific protocols. It is therefore important that the clinician understand the mechanism by which the most commonly used bronchoprovocation testing works. It is important that the clinician understand the mechanism of action in the testing, whether direct stimuli (methacholine) or indirect stimuli (mannitol, exercise) is implemented, when the testing is performed and the results interpreted.
Introduction
Nonspecific bronchoprovocation test is an important test for diagnosing asthma by measuring airway hyperresponsiveness123, consists of direct bronchoprovocation test with high sensitivity and low specificity, and indirect bronchoprovocation test with low sensitivity and high specificity, respectively1.
1. Asthma and bronchoprovocation test
Bronchial asthma is a disease characterized by airway hyperresponsiveness that airway narrows by airway inflammation and various inducing stimulus14. Since the airway hyperresponsiveness is caused by inflammation of airway, the degree is proportional to severity of asthma, and reduced by the treatment1456. Therefore, measuring the airway hyperresponsiveness is important in diagnosing the asthma, assessing the severity, and determining the response to treatment. Methods for measuring the airway hyperresponsiveness can be largely divided into the method for observing an improvement of airflow limitation by bronchodilator, and the bronchoprovocation test in which airflow limitation is induced by pharmacologic or non-pharmacologic stimuli789.
2. Indications and contraindications of bronchoprovocation test
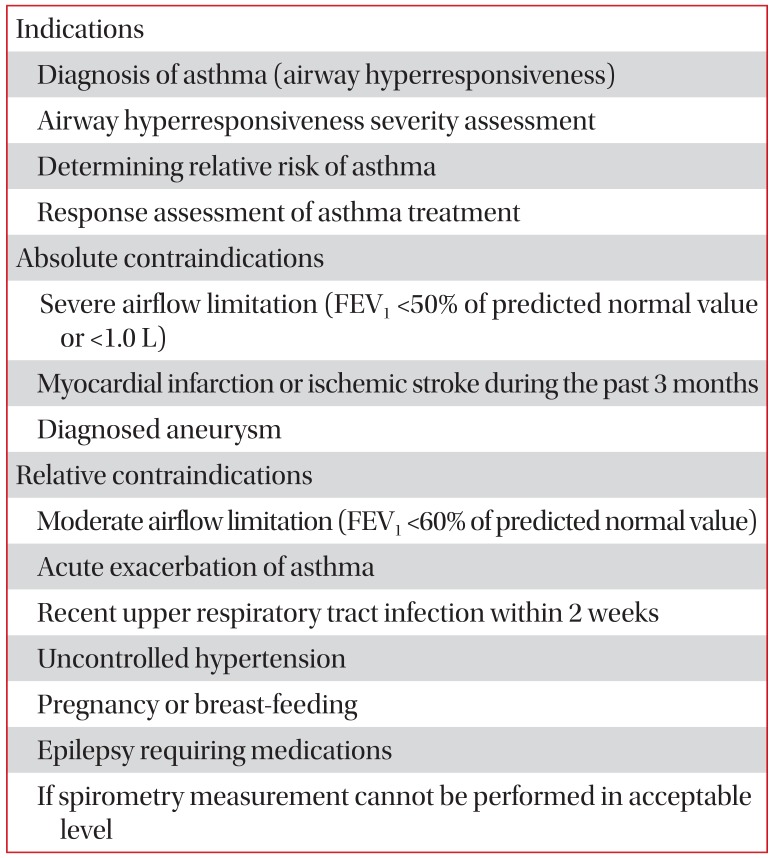
Indications and contraindications of the bronchoprovocation test are represented (Table 1)12.
3. Types of nonspecific bronchoprovocation test
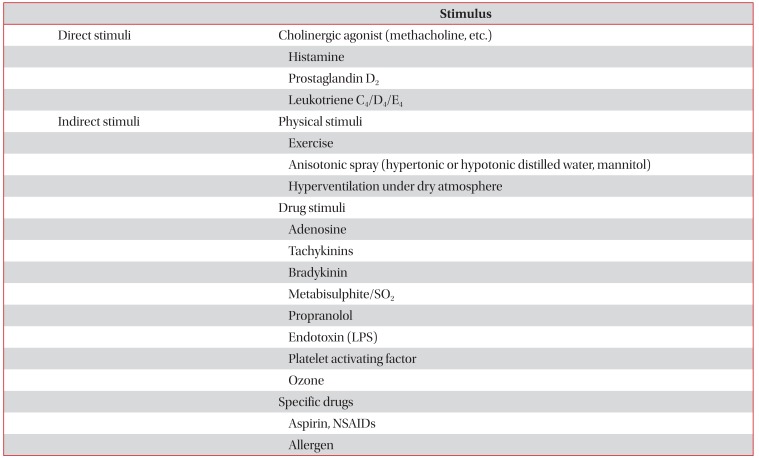
Nonspecific bronchoprovocation test is performed using a number of inducing stimuli, and there are advantages and disadvantages. Direct bronchoprovocation test using methacholine or histamine is very sensitive since it directly stimulates airway smooth muscle cells, but it also has a disadvantage of low specificity. However, because the indirect bronchoprovocation test using mannitol, exercise, hypertonic saline, adenosine, and hyperventilation cause reactions in airway smooth muscle cells by liberating mediators with stimulation of airway inflammatory cells other than the airway smooth muscle cells, airway epithelial cells and nerves; although it shows low sensitivity but has an advantage of high specificity78910. The direct and indirect stimuli are represented (Table 2)7911.
1) Direct bronchoprovocation test
Direct bronchoprovocation test is particularly useful to rule out the diagnosis of asthma due to high sensitivity. In contrast, because of the disadvantage of low specificity, it is hard to evaluate the clinical significance even if the test result is positive. Methacholine, as a muscarinic agonist, has a high diagnostic value to the patient with high probability of asthma on pre-test7810.
Methacholine Provocation Test
1. Introduction
Methacholine provocation test is one method for measuring the airway hyperresponsiveness, and airway hyperresponsiveness is one of the features that can help in the diagnosis of asthma. Even though it can vary depending on the time, typically increases in exacerbation but deceases during the treatment with anti-inflammatory drugs212.
Methacholine provocation test, as traditional methods that is frequently considered on high likelihood of asthma, is more useful to rule out the diagnosis of asthma than to diagnose the asthma. This is because the negative predictive power is higher than the positive predictive power212.
2. Indications
Methacholine provocation test is a useful tool to assess the occupational asthma. In addition, it can also be used to determine the relative risk of asthma, even though a clinical significance is not yet established clearly, it can used to assess the response to treatment of asthma2.
In patients with moderate possibility of asthma, results of the methacholine provocation test cannot be predicted accurately, even if by the asthma specialists. Methacholine provocation test has very excellent sensitivity for asthma, but positive predictive power is relatively poor2.
Most people with asthma symptoms have the bronchial hyperresponsiveness. However, bronchial hyperresponsiveness may be observed in other diseases, such as chronic obstructive pulmonary disease (COPD), congestive heart failure, cystic fibrosis, bronchitis or allergic rhinitis2.
Because clinical improvement of asthma is associated with improvement in airway hyperresponsiveness, clinical asthma research often used the change of airway hyperresponsiveness as an objective result index. However, the use of the methacholine provocation test in the clinical evaluation of asthmatic patients will have to wait for additional research on the usefulness of the test2.
3. Contraindications
Contraindications of the methacholine provocation test is the same as the contraindications of general bronchoprovocation tests mentioned in the “Introduction,” and cases of current using of cholinesterase inhibitors (in case of myasthenia gravis) specifically are included in the contraindications. In other words, all the situations that may decrease a quality of test or increase risk and discomfort of patients are included; therefore, these points should be identified through interviews or questionnaires before the test. If the contraindication is confirmed, it is necessary to consult with a medical doctor or a laboratory director before conducting the test23.
Rapid reduction in forced expiratory volume at 1 second (FEV1) can occur sometimes during the methacholine provocation test, this risk occurs frequently in people who have low baseline lung function. But because even worse lung function has the low risk of serious side effects, low lung function is a relative contraindication of the methacholine provocation test. There is controversy about the level of lung function that is contraindications of the methacholine provocation test. Typically, the basal FEV1 <1.5 L or predicted normal value <60% in adults are used as a relative contraindication, The National Asthma Expert Panel Report 2nd edition has recommended FEV1 <65% as a relative contraindication23.
1) Airway obstruction
Because airway responsiveness shows a strong correlation with the degree of basal airway obstruction in COPD, positive methacholine provocation test can be difficult to interpret. If there are the clinical aspects consistent with asthma, airway obstruction at baseline spirometry test and significant bronchodilator response (FEV1 or forced vital capacity >12% and increase >0.2 L), these can be confirmed as asthma and the methacholine provocation test is not necessary23.
2) The quality of spirometry tests
The methacholine provocation test of acceptable level depends on the patient's ability to perform an appropriate spirometry test. Patients unable to perform the appropriate spirometry test on baseline step should reschedule a test or consider other diagnostic methods23.
3) Cardiovascular disease
History of cardiovascular disease may also be a contraindication. Additional cardiovascular stress by the induced airway constriction may exacerbate the cardiovascular problem in the patients with history of uncontrolled hypertension or recent heart attack and stroke. If the airway constriction is induced, it becomes the cause of ventilation-perfusion imbalance that can result in arterial hypoxia and changes in blood pressure, cardiac output and heart rate.
4) Pregnancy and breast-feeding
Methacholine is a pregnancy category C drug. It is not yet known whether methacholine is excreted in breast milk23.
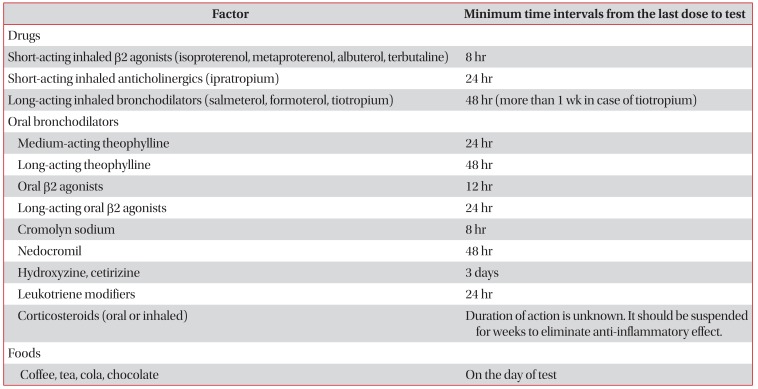
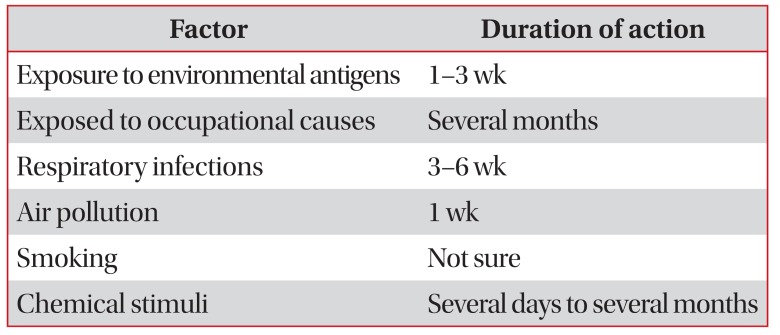
Drugs or conditions represented in Table 3 should be avoided before methacholine provocation test2. Because these factors decrease airway reactivity, it should be stopped by each time interval before the test. Table 4 is represented the factors that may increase the airway reactivity2.
4. Interpretations
FEV1 most commonly used as bronchoprovocation test results, is easy to test and shows excellent reproducibility. When the dose-response curve is obtained with inhaled drug concentration and FEV1, the inhaled drug concentration is represented on X-axis as log scales and the reduction ratio of FEV1 is represented on Y-axis as numbers, respectively. Methacholine concentration at the point that FEV1 is decreased to 20% of baseline in the dose-response curve is called PC20 (provocation concentration causing a 20% fall in FEV1), and it is regarded as an index of the bronchial hyperresponsiveness2.
If PC20 is less than 1.0 mg/mL, specificity and positive predictive value almost close to 100%, so that the diagnosis of asthma can be confirmed. If PC20 is less than 8–16 mg/mL, it is considered to have airway hyperresponsiveness. If PC20 is not less than 10 mg/mL, it is very likely that there is no apparent asthma21314.
Since the effect is shown by the accumulation of the dose from the start of inhalation in the methacholine provocation test, it is also represented by using a accumulated dose instead of the density, and the accumulated dose of methacholine to the point that the bronchoconstriction is induced may appear as PD20 (provocation dose causing a 20% decline in FEV1)215.
Mannitol Provocation Test
Mannitol provocation test is a type of indirect provocation test, which has high specificity and the advantages of being simple and safe, but low sensitivity. If FEV1 is decreased by 15% or more compared to baseline with 635 mg or less of mannitol, it is determined that airway hyperresponsiveness to the mannitol is shown31617.
1. Introduction
Mannitol provocation test, which is a type of indirect bronchoprovocation tests, is to access the reaction acting on airway smooth muscles cells by liberating mediators with stimulation of inflammatory cells91617.
It has higher specificity than the methacholine provocation test on the diagnosis of asthma, and it is closely related to eosinophilia or increased exhaled nitric oxide (eNO) levels, which reflect the inflammatory status of airway71718. Therefore, if the mannitol provocation test is positive in a patient with symptoms that asthma can be suspected, it means that there is asthma accompanied by progressive airway inflammation, and it may determine that the anti-inflammatory treatment is necessary.
Mannitol provocation test has the advantages of high specificity and being simple and safe, while there are disadvantages of relatively low sensitivity that only about 60% of asthma patients can be found31619. Therefore, negative mannitol provocation test cannot rule out the asthma.
Although methacholine, histamine, etc. induce bronchoconstriction by directly stimulating the bronchial smooth muscle receptors, indirect stimuli such as hypertonic saline, exercise, adenosine, mannitol stimulate mast cells etc. to secrete inflammatory mediators, then these mediators cause a contraction of bronchial smooth muscles by acting as strong bronchoconstrictors, which result in a reduction of the inner diameter of bronchus91617. Mannitol is not absorbed into the body as sugar alcohols (C6H6(OH)6), thus it remains in the airway surface when inhaled into the airway and increases the osmotic pressure. Water in the cells is moved out of the cells by the osmotic pressure difference, which results in cellular contraction316.
2. Interpretations
If FEV1 is decreased by 15% or more compared to baseline with 635 mg or less of accumulated mannitol dose in the repeated tests, it is determined that airway hyperresponsiveness to the mannitol is positive31617.
PD15 is defined as the mannitol dose (mg) which is inhaled until the time when FEV1 is reduced by 15% of baseline31720.
Response dose ratio (RDR) is defined as FEV1%/mannitol dose (mg) of the time when FEV1 is decreased by 15% of baseline. If FEV1 is reduced by 15% compared to the baseline after using mannitol 635 mg, it is denoted by PD15 635 mg, RDR 0.024%/mg (15%/635 mg)1620.
Because the mannitol provocation test means asthma caused by eosinophilic airway inflammation and shows moderate sensitivity (60%), well-controlled asthma, mild asthma, non-eosinophilic asthma can show negative results1619. In addition, if the test time exceeds 35 minutes or the excessive movement is performed before the test, test result may be false negative and it is known that smoking and chronic cough increase the response to the mannitol916. If the mannitol provocation test is performed in the normal group, FEV1 reduction usually does not exceed 10%91621.
Although about 83% of examinee experiences cough during the test, severe cough enough to stop the test only occurs in 1.3%3162022. The other side effects may appear such as headache (6.1%), sore throat (2.6%)31620.
Exercise Provocation Test
Exercise provocation test is an indirect provocation test to determine the occurrence of nonspecific airway hyperresponsiveness by airway cooling and drying12. Contraindications and prior stopped drugs of the exercise provocation test are the same as the bronchoprovocation test12. Exercise provocation test is performed using a treadmill or bicycle ergometer, in accordance with the appropriate protocol in safe facilities and personnel conditions. If decrease by 15% and more of baseline FEV1 is induced, it is determined as positive123.
1. Introduction
Exercise induces airway constriction in the majority of patients with asthma, exercise-induced airway contractions is called as exercise-induced asthma or exercise-induced bron-choconstriction (EIB)123.
There are ventilation by exercise and moisture content and temperature of the inhaled air as the main factors that determine the severity of the EIB, and if the large amount of air loses the moisture in a short time due to the exercise, the airway contraction occurs by osmotic effects caused by temperature changes (cooling and re-heating) and dehydration12323.
Airway cooling and drying are considered to stimulate the liberating of inflammatory mediators such as histamine and leukotriene, eventually the exercise itself is also an important provocation test to evaluate the effect of the anti-inflammatory agents and other asthma prescription1232425.
2. Indications
It is used as a provocation test for the diagnosis of EIB in the asthma patient with a history of shortness of breath during or after exercise12.
The EIB test is required if working ability is impaired due to suspected asthma symptoms associated with exercise in certain occupational groups (occupations to deal with emergency situations such as armed forces, police, firefighting)22627.
It is used to determine the effectiveness and optimum dose of drugs that are prescribed to prevent the EIB, and to evaluate acute (such as cromolyn sodium and nedocromil sodium) or chronic (steroid and leukotriene antagonists) anti-inflammatory effects of the treatment2.
3. Contraindications
Contraindications are the same as the general bronchoprovocation tests mentioned in the “Introduction”12. In addition, the test should not be performed in cases of the unstable ischemic heart disease or malignant arrhythmia123.
In case of the orthopedic problems, an appropriate degree of exercise to induce airway contraction is likely not to be performed. 12-Lead electrocardiogram recorded during the last year should be checked in patients aged 60 or more2.
4. Interpretations
FEV1 is the primary variables for reactive evaluations, and spirometry test to measure these should be proceeded in the sitting position continuously before and after exercise123.
Appropriately measured values should be obtained for each test times at least 2 times or 3 times if possible, and difference between the highest and second highest FEV1 should be within 0.2 L. The highest value of the valid FEV1 is selected as a representative value of each test time2.
Expiratory time should be limited to 2–3 seconds; it is very important to lead very aggressively the patients to breathe in as deeply as possible in all cases2.
EIB is determined by converting the measured FEV1 at each time after exercise to % of baseline FEV1 before exercise, and the case that is reduced to 90% of the baseline FEV1 is regarded as the general abnormal response12. The decrease of FEV1 by 15% and more is considered a more diagnostic value to the EIB, especially the exercise provocation test is performed outdoors228.
Conclusion
Nonspecific bronchoprovocation test is an important test for diagnosing asthma by measuring the airway hyperresponsiveness, and includes direct (methacholine) and indirect (mannitol, exercise) bronchoprovocation test. The tests need descriptions of specific measurement conditions, such as the selection of subjects, the choice of the stimulus, the method of measurement of bronchoconstriction, and technical or medical precautions. In addition, it has become evident that challenge tests with each of the various bronchoconstrictors stimuli require distinct protocols. Therefore, it is important to understand the most commonly used bronchoprovocation tests with direct stimuli and indirect stimuli when we perform the tests and interpret the results.
Notes
Conflicts of Interest: No potential conflict of interest relevant to this article was reported.