 |
 |
| Tuberc Respir Dis > Volume 78(4); 2015 > Article |
|
Abstract
Gastric mucosal damage by iron pills is often reported. However, iron pill aspiration is uncommon. Oxidation of the impacted iron pill causes bronchial mucosal damage that progresses to chronic bronchial inflammation, necrosis, endobronchial stenosis and rarely, perforation. We reported a case of a 92-year-old woman with chronic productive cough and significant left-sided atelectasis. Bronchoscopy revealed substantial luminal narrowing with exudative inflammation of the left main bronchus. Bronchial washing cytology showed necroinflammatory exudate and a small amount of brown material. Mucosal biopsy showed diffuse brown pigments indicative of ferrous pigments, crystal deposition, and marked tissue degeneration. After vigorous coughing, she expectorated dark sediments and her symptoms and radiological abnormalities improved. There are a few such reports worldwide; however, this was the first case reported in Korea. Careful observation of aspiration-prone patients and early detection of iron pill aspiration may prevent iron pill-induced bronchial injury.
Iron pills are frequently prescribed to treat iron deficiency anemia. The elderly, pregnant women, and children and patients who have gag reflex problems or swallowing difficulty are high-risk groups for aspiration1. There are a few reports indicating that iron pill aspiration leads to bronchial necrosis and stenosis2,3. We encountered a case of bronchial mucosal damage and resultant atelectasis associated with the aspiration of an oral iron pill.
A 92-year-old woman visited our clinic after experiencing cough and expectoration of brown sputum for a few weeks. She had dyspnea (Modified Medical Research Council Dyspnea Scale [MMRC] grade 3), but she did not complain of fever or myalgia. She had been receiving long-term treatment for hypertension, Parkinson's disease and chronic kidney disease. Because of iron deficiency anemia, she was treated with oral iron pills (Feroba-U, a brown round tablet, containing ferrous sulfate 256 mg, ascorbic acid 30 mg, and L-glutamine 30 mg), which she took for 3 months daily after breakfast. She had recently experienced occasional aspiration of her medications.
The patient was alert and the following findings were noted in the physical examinations on admission: blood pressure, 120/70 mm Hg; pulse rate, 74 beats per minute; respiratory rate, 18 breaths per minute; and body temperature, 36.4Ōäā. She had a chronic ill appearance. Her conjunctiva was not anemic and her sclera was not icteric. Dull breath sounds with end-inspiratory and expiratory wheezing were auscultated on the left lung field. The heart beats were regular without murmur at auscultation. Her face and extremities were not edematous on physical examination.
A chest radiograph showed near total atelectasis and a suspiciously large amount of pleural effusion in the left mid and lower lung fields (Figure 1A). In the chest computed tomography (CT) images, near total atelectasis of the left lung and a dense calcified nodular material impacted at the left main bronchus were visible, which suggested obstructive pneumonia with atelectasis due to foreign body impaction (Figure 2). The image also showed subsegmental atelectasis in the right middle lobe and the right lower lobe anterior basal segment with a large bullous lesion in the right middle lobe medial segment, which suggested a post-inflammatory lesion.
The laboratory test findings were as follows: white blood cell count, 10,100/mm3 (the fraction of segmented cells was 78.1%); hemoglobin, 9.2 g/dL; platelet count, 216,000/mm3; aspartate aminotransferase, 19 IU/L; alanine aminotransferase, 13 IU/L; total bilirubin, 0.2 mg/dL; blood urea nitrogen, 32 mg/dL; creatinine, 1.7 mg/dL; total protein, 6.1 g/dL; albumin, 3.2 g/dL; lactate dehydrogenase, 385 U/L; C-reactive protein, 1.20 mg/dL (0.1-0.8 mg/dL); creatinine kinase-MB, 3.2 ng/mL (0.3-4 ng/mL); troponin-I, 0.03 ng/mL (0-0.1 ng/mL); brain natriuretic peptide, 330 pg/mL; and prothrombin time/international normalized ratio, 0.89. Arterial blood gas analysis on room air showed a pH of 7.36, a PaO2 of 65.9 mm Hg, and a PaCO2 of 27.9 mm Hg. Pleural fluid analysis showed the following findings: pH, 7.0; red blood cell count, 40/mm3; white blood cell count, 130/mm3; polymorphonuclear cells, 12%; mononuclear cells, 88%; protein, 2.9 g/dL; albumin, 1.8 g/dL; lactate dehydrogenase, 161 U/L; and glucose, 124 mg/dL. According to Light's criteria, this indicated transudate.
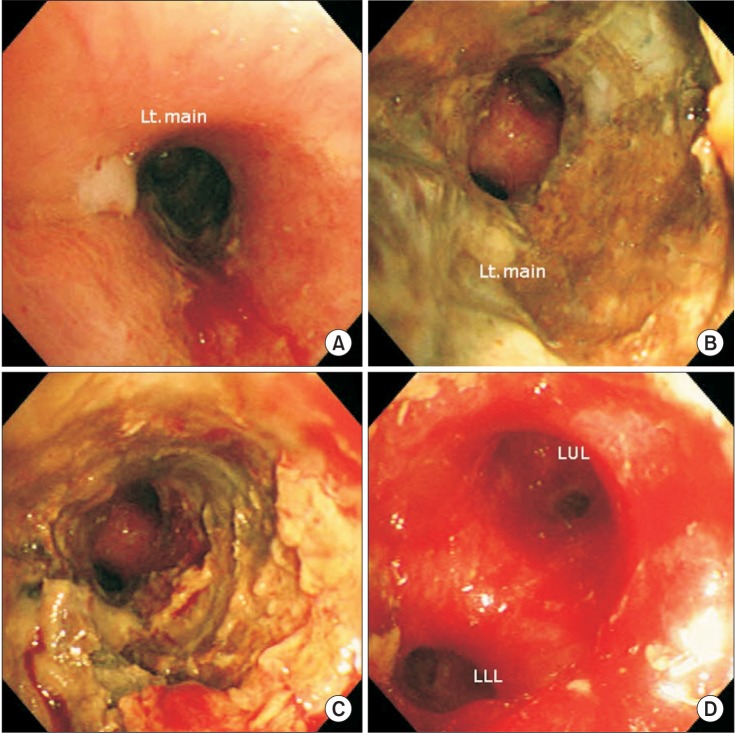
On the third hospital day, one-half of a smothered oral pill was disgorged after severe coughing. One day later, the chest radiograph showed remarkably improved atelectasis and decreased pleural effusion (Figure 1B). On the fifth hospital day, bronchoscopy was performed to investigate suspicious endobronchial lesion. The bronchoscopic results were as follows: the proximal portion of the left main bronchus was substantially narrow with nodular mucosal changes (Figure 3). During the procedure, even a very light touch caused significant mucosal bleeding. The distance between the nodular mucosal lesion and the carina was approximately 2 cm. The distal portion of the left main bronchus could not be clearly examined because of significant mucosal bleeding. However, from the distal portion, the lumen of the left upper lobe and the left lower lobe seemed to be intact.
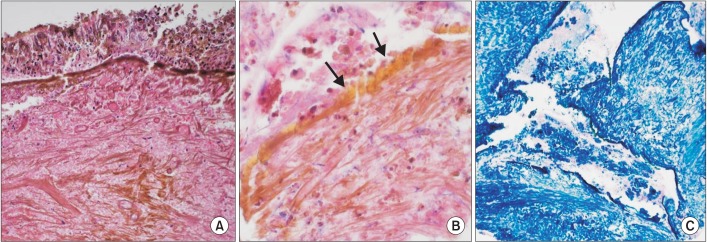
Bronchial washing cytology revealed necroinflammatory exudates and a small amount of brown material. The mucosal biopsy from the left main bronchus microscopically showed marked tissue necrosis and degeneration with diffuse golden-yellow and brown pigments and crystal deposition (Figure 4A, B). Prussian blue stain (i.e., iron staining) was diffusely and strongly positive in the biopsied tissue, especially in the brown pigment and in the crystals, which confirmed the presence of ferric iron (Figure 4C). Based on the clinical history, bronchoscopic findings, and microscopic features, we concluded that the patient's disease was iron pill-induced mucosal damage in the left main bronchus and resultant atelectasis of the left lung. She was treated conservatively with antibiotics for a significant amount of purulent sputum and mucosal inflammation. The patient's symptoms, which included dyspnea and cough, and atelectasis on chest radiograph improved thereafter. We recommended that she should quit taking iron pills for a while and undergo repeated blood tests for anemia later. After discharge, she had no aggravated respiratory symptoms during 6 months of follow-up.
Iron pill-induced injury in the gastrointestinal tract is well known. It is characterized by a variable combination of mucosal ulceration and erosion, acute inflammation with luminal inflammatory exudates, and granulation tissue4. However, patients with iron pill aspiration to the respiratory tract are uncommon and occasionally reported. The reason iron pills are more easily aspirated than other drugs is very unclear; however, the shape and size of the iron pill tablets and the characteristics of patients who take iron pills may influence the possibility of aspiration3.
Delgado-Sanchez et al.5 demonstrated iron pill-induced bronchitis, which caused iron deposition at the bronchial mucosa and mucosal inflammation. Bronchial stenosis might be also caused by the progression of iron pill-induced bronchitis. In severe cases, iron pill bronchitis could be fatal because it may lead to perforation of the bronchus. After several years, granulation tissue forms slowly and may lead to the bronchial obstruction and fibrosis. Persistent bronchial stenosis may sometimes require specific local treatments such as lobectomy or bronchoplasty3. According to Lee et al.6, bronchial mucosal changes after iron pill aspiration represents a syndrome. And, it was also reported as a spectrum that ranges from acute mucosal damage to granulation tissue formation7.
Our patient was a 92-year-old woman who had Parkinson's disease for several years and complained of recent swallowing difficulty and general weakness. Patients with swallowing difficulty should take iron pills carefully because of the risk of aspiration and possible endobronchial damage. Iron pill aspiration is more dangerous than other foreign body aspiration because of acute chemical injury caused by the induction of cytotoxic oxidant radicals. Oxidation of the tablet begins immediately after its direct contact with the bronchial mucosa8. Therefore, it is important that the iron pill is quickly removed from the bronchus to prevent subsequent endobronchial damage in patients with iron pill aspiration.
The definitive diagnostic method for iron pill bronchitis is bronchoscopy with mucosal biopsy. Bronchoscopic findings of iron pill aspiration are reportedly a golden-yellow mucosal change and mucosal inflammation, necrosis, ulceration, or sloughing9. In addition to the brown material at the bronchial wall and mucosal inflammation revealed by bronchoscopic biopsy, some patients have fibrotic changes and granulation tissue. Iron deposition could also be identified by a positive response to Prussian blue stain.
In our patient, we initially suspected a malignant lesion because of the severe nodular mucosal change in the proximal left main bronchus and resultant atelectasis of the left lung. However, from the biopsy specimen, we only noticed small or moderate amounts of hemosiderin within the macrophages instead of tumor cell infiltration in the deep-layered mucosal change. Because of the patient's history of recently repeated aspiration just after taking oral medications and the results of bronchoscopic mucosal biopsy, we could confirm the diagnosis of oral iron pill-induced bronchitis.
To prevent iron pill-induced bronchitis, some authors recommend that patients with swallowing difficulties should take iron syrup instead of iron pills5. A good prognosis could also result if the iron pill is removed quickly through bronchoscopy, after the pill has been aspirated. Furthermore, removing the tablet should clearly be attempted wherever possible to minimize tissue damage and subsequent complications.
This case report is the first in Korea, although there are a few reports worldwide. We could discover and confirm an oral iron pill as a calcified nodular lesion at the left main bronchus on chest CT imaging. This case report is meaningful because endobronchial injury due to iron pill aspiration happens very infrequently. The patient's symptoms and radiological abnormalities rapidly improved after she expectorated the oral iron pill.
Iron tablets may be prescribed frequently for elderly patients, in whom anemia is very common and the risk of aspiration due to various underlying diseases is not negligible. The possibility of iron pill aspiration in "aspiration-prone" patients should be considered at the beginning of iron pill prescription in high-risk patients. If iron pill aspiration is documented or even suspected, immediate evaluation of iron pill-induced bronchitis and removal of the iron pill, when possible, should be considered. In conclusion, cautious observation of aspiration-prone patients and early detection of iron pill aspiration may be important to prevent iron pill induced bronchial injury.
References
1. Hill SN, Main AN, Fuggle WJ. Covert inhalation of tablet causing fatal pneumonia. Postgrad Med J 1988;64:66-67. PMID: 3420061.



2. Tarkka M, Anttila S, Sutinen S. Bronchial stenosis after aspiration of an iron tablet. Chest 1988;93:439-441. PMID: 3276459.


3. Lamaze R, Trechot P, Martinet Y. Bronchial necrosis and granuloma induced by the aspiration of a tablet of ferrous sulphate. Eur Respir J 1994;7:1710-1711. PMID: 7995402.


4. Cimino-Mathews A, Illei PB. Cytologic and histologic findings of iron pill-induced injury of the lower respiratory tract. Diagn Cytopathol 2013;41:901-903. PMID: 22508539.


5. Delgado-Sanchez L, Atwal P, Krishnan P. Iron pill induced bronchitis. Int J Case Rep Imag 2012;3:34-36.

6. Lee P, Culver DA, Farver C, Mehta AC. Syndrome of iron pill aspiration. Chest 2002;121:1355-1357. PMID: 11948075.


7. Godden DJ, Kerr KM, Watt SJ, Legge JS. Iron lung: bronchoscopic and pathological consequences of aspiration of ferrous sulphate. Thorax 1991;46:142-143. PMID: 2014497.



8. Aust SD, Morehouse LA, Thomas CE. Role of metals in oxygen radical reactions. J Free Radic Biol Med 1985;1:3-25. PMID: 3013969.


9. Kim ST, Kaisar OM, Clarke BE, Vandenburg RA, Allen DH, Bell SC, et al. 'Iron lung': distinctive bronchoscopic features of acute iron tablet aspiration. Respirology 2003;8:541-543. PMID: 14708558.


Figure┬Ā1
(A) At admission, chest radiograph shows near total atelectasis of the left lung and a large amount of pleural effusion in the left hemithorax. (B) On the fifth hospital day, chest radiograph reveals clear overall lung field with improved atelectasis and decreased effusion.

Figure┬Ā2
Chest computed tomography images show near total atelectasis of left lung and a dense calcified nodular lesion (arrow) impacted at the left main bronchus.

- TOOLS
-
METRICS

- Related articles
-
A case of bronchial obstruction due to occult aspiration of a tooth.1993 August;40(4)
A Case of the Bronchial Artery-Pulmonary Vein Malformation.1995 October;42(5)
A Case of Pneumonia due to Occult aspiration of a Twig.1996 February;43(1)
A Case of Hodgkins Disease as Endobronchial Presentation.1998 June;45(3)


 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Print
Print Download Citation
Download Citation



