 |
 |
| Tuberc Respir Dis > Volume 73(3); 2012 > Article |
|
Abstract
Background
The release of interferon-gamma (IFN-╬│) by T lymphocytes increases after rechallenge with Mycobacterium tuberculosis antigen, especially, at a localized site of tuberculosis (TB) infection. We aimed to compare the clincial efficacy of two commercial IFN-╬│ release assays from pleural fluid for the diagnosis in tuberculous pleurisy.
Methods
We performed T-SPOT.TB and QuantiFERON-TB Gold tests simultaneously on pleural fluid and peripheral blood samples from patients with pleural effusion, in South Korea, an area with intermediate TB burden.
Results
Thirty-six patients were enrolled prospectively, and tuberculous pleurisy was found in 21 patients. Both the numbers of IFN-╬│ secreting T cells and the concentration of IFN-╬│ were greater in the pleural tuberculous group, comparing with the non-tuberculous group. Moreover, in the tuberculous group, there was a significant difference in IFN-╬│ producing spot-forming cells using the T-SPOT.TB method between pleural fluid and peripheral blood. The receiver operating characteristic (ROC) curve, was the greatest for pleural fluid T-SPOT.TB test, followed by peripheral blood T-SPOT.TB test, peripheral blood QuantiFERON-TB Gold test, and pleural fluid QuantiFERON-TB Gold test (area under the ROC curve of 0.956, 0.890, 0.743, and 0.721, respectively). The T-SPOT.TB assay produced less indeterminate results than did QuantiFERON-TB Gold assay in both pleural fluid and peripheral blood.
Tuberculous pleurisy is a common extrapulmonary form of tuberculosis (TB) worldwide and also is the most common manifestation in South Korea1. However, tuberculous pleurisy is frequently difficult to confirm because existing diagnostic approaches, such as pleural tapping and biopsy, are relatively invasive and the results require much time and have variable sensitivity2-5.
In the late 1990s, research on the Mycobacterium tuberculosis genome led to the identification of early secretory antigenic target-6 (ESAT-6) and culture filtrate protein-10 (CFP-10), which appear exclusively in M. tuberculosis (i.e., not in M. bovis Bacillus Calmette-Gu├®rin vaccine or most environmental nontuberculous mycobacteria)6,7. Based on the finding that T lymphocytes that are exposed to M. tuberculosis release more interferon-╬│ (IFN-╬│) cytokine on repeat exposure to these specific antigens, T-cell-based IFN-╬│ release assays (IGRAs) have been developed and are approved for diagnosis of latent TB by US and European Union6-8. Two tests, the T-SPOT.TB assay (Oxford Immunotec, Oxford, UK) and QuantiFERON-TB assay (Cellestis, Carnegie, Australia), are commercially available. These two methods differ mainly in their techniques for IFN-╬│ detection (ELISPOT vs. enzyme-linked immunosorbent assay [ELISA]) and the specimens used (mononuclear cells vs. whole blood).
During active TB, mycobacterium-specific T cells proliferate and are recruited to the site of infection9,10. Recognizing this phenomenon and using M. tuberculosis-specific antigen, Jafari et al.11 demonstrated that active pulmonary TB can be confirmed rapidly with an ELISPOT assay in bronchoalveolar lavage fluid in smear-negative setting. In tuberculous pleurisy, more CD4+ T lymphocyte subgroups are found in the pleural fluid (PF) than in peripheral blood (blood), and more IFN-╬│ is secreted by T lymphocytes in the PF than in blood9. Therefore, we investigated the clinical utility of two IGRAs applied to both PF and blood obtained from patients with pleural effusion for the diagnosis of tuberculous pleurisy.
During the 9-month period from December 2007 to August 2008, consecutive adult patients who visited Yeouido St. Mary's Hospital (Seoul, Korea) with unilateral pleural effusion were enrolled prospectively in the study after providing written consent. The Institutional Review Board of Yeouido St. Mary's Hospital approved this study. All patients were asked about their past TB history, clinical symptoms, and radiologic findings. Thoracentesis was performed in every patient, and a pleural biopsy was performed if possible. PF, pleural tissue, and sputum specimens were subjected to routine biochemical, microbiological, and histological evaluation. Tuberculous pleurisy was diagnosed if any of the following criteria was met: 1) positive results for a TB culture, acid-fast bacilli or TB polymerase chain reaction from the respiratory specimens; 2) histological analysis of the pleural tissue showing granulomatous inflammation with or without caseous necrosis or multinucleated giant cells; or 3) pleural effusion comprising lymphocyte-dominant exudates with adenosine deaminase concentration >40 U/L and a positive treatment response to 6 months of antituberculous therapy and if no alternative diagnosis for the effusion other than TB was appropriate, according to a previous study12. We used the definition of an immunocompromised condition as provided by Lee et al.13. The tuberculin skin test was performed using the Mantoux test as described previously14. Patients younger than 18 years of age and whose cause of effusion was not identified were excluded from the study.
We collected blood and PF on the same day and all patients except one did not take the antituberculous medication before sampling. We performed the two IGRAs, T-SPOT.TB test and QuantiFERON-TB Gold (QFT-G) test on blood samples following the manufacturers' instructions. For the T-SPOT.TB assay in PF, we transferred PF to a Falcon tube; the tube was centrifuged, and mononuclear cells (Ōēź1├Ś107) were separated within 2 hours after thoracentesis. To collect an adequate numbers of the cells, we used sufficient amounts, more than 50 mL of PF. The T-SPOT.TB assay was performed on 2.5├Ś105 cells per well. The subsequent processes were the same as for the test using blood samples. For the QFT-G test, 1 mL of PF was collected in the tubes supplied containing the M. tuberculosis-specific antigens ESAT-6 and CFP-10, nil control, or a mitogen control (phytohemagglutinin). The tubes were incubated within 5 hours of collection for 18 hours at 37Ōäā and then centrifuged. The supernatants were stored at -80Ōäā until the ELISA was performed.
We interpreted the results of the IGRAs on blood as recommended for each test. The results of the T-SPOT. TB test were considered indeterminate if the spot number of nil control was >1013. The results of the QFT-G assay were considered indeterminate if one of the following occurred: the nil value was >8 IU/mL; when if the nil value was Ōēż8 IU/mL, the TB antigen minus the nil value was <0.35 or it was Ōēź0.35 and <25% of the nil value, and the mitogen value minus the nil value was <0.514. To assess the diagnostic accuracy, we plotted receiver operating characteristic (ROC) curves among the IGRAs. We recalculated new best cut-off values of the tests (T-SPOT.TB and QFT-G) by applying simplified diagnostic criteria which are the difference in the counts of spot-forming cells and in the concentrations of IFN-╬│ between antigen stimulated samples and the negative control, respectively, without considering the indeterminate results.
The results for each group were compared using the Mann-Whitney U test in SPSS version 12.0 (SPSS Inc., Chicago, IL, USA). We constructed a ROC curve by plotting the rate of sensitivity against the rate of (1-specificity) results over a range of cutoff values of T-SPOT.TB and QFT-G test performed on blood and PF. A p-value of <0.05 was considered significant.
Of the 36 patients with undetermined unilateral pleural effusions, 21 were diagnosed as tuberculous pleurisy. Their average age was 49.7 years (range, 19~89 years). Age differed significantly between the tuberculous group and non-tuberculous group (Table 1). The patients were tested for human immunodeficiency virus (HIV) antibodies, and all were negative. In the tuberculous group, no patient had any immunocompromising disease, and in the non-tuberculous group, one patient was undergoing hemodialysis. The Mantoux test results were available in 25 patients; 15 were in the tuberculous group and five were positive. A pleural biopsy was performed in 25 of 36 patients, and 18 were in the tuberculous group. Tuberculous pleurisy was diagnosed by microbiological, histological, and biochemical/clinical criteria in 12 patients, six patients, and three patients, respectively. The common causes of the non-tuberculous pleurisy were malignancy (n=7), parapneumonic effusion (n=3), and heart failure (n=3). The serum albumin level, a nutritional marker, and the lymphocyte count in blood and PF did not differ between the tuberculous and nontuberculous groups.
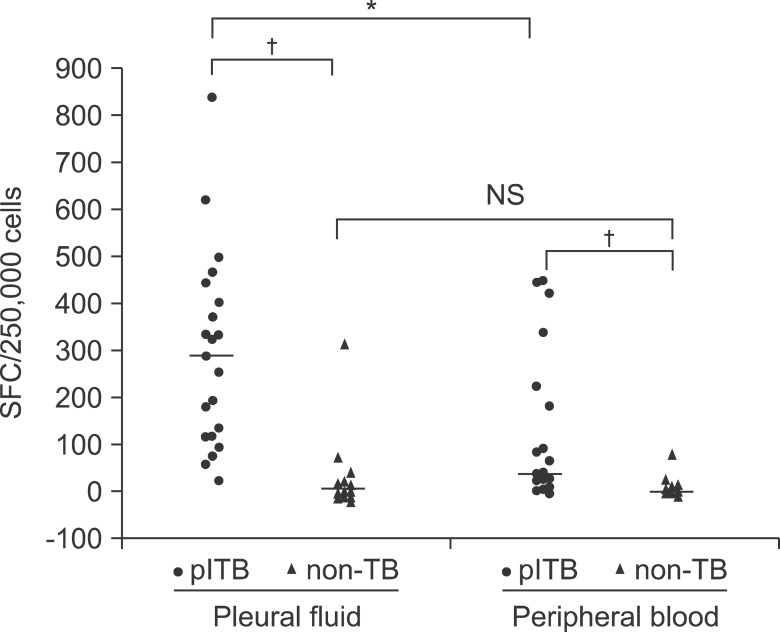
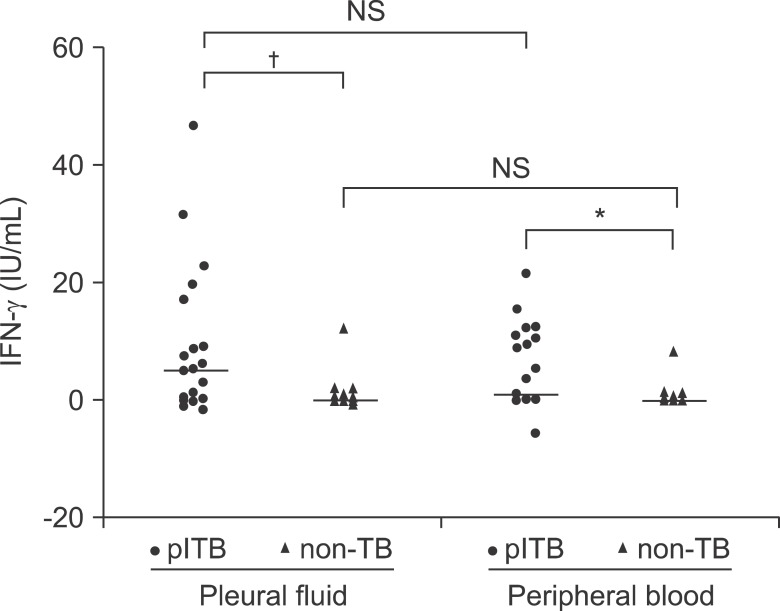
Compared to the nontuberculous group, the tuberculous group had significantly more spot-forming T cells in both PF and blood. Within the tuberculous group, there were more immunospots in the T-SPOT.TB assay in PF than in blood (Figure 1). In the QFT-G test in PF and blood, the IFN-╬│ response was significantly higher in the tuberculous patients than in the non-tuberculous patients. However, within the tuberculous group, the QFT-G assay detected no difference in the IFN-╬│ response between PF and blood (Figure 2).
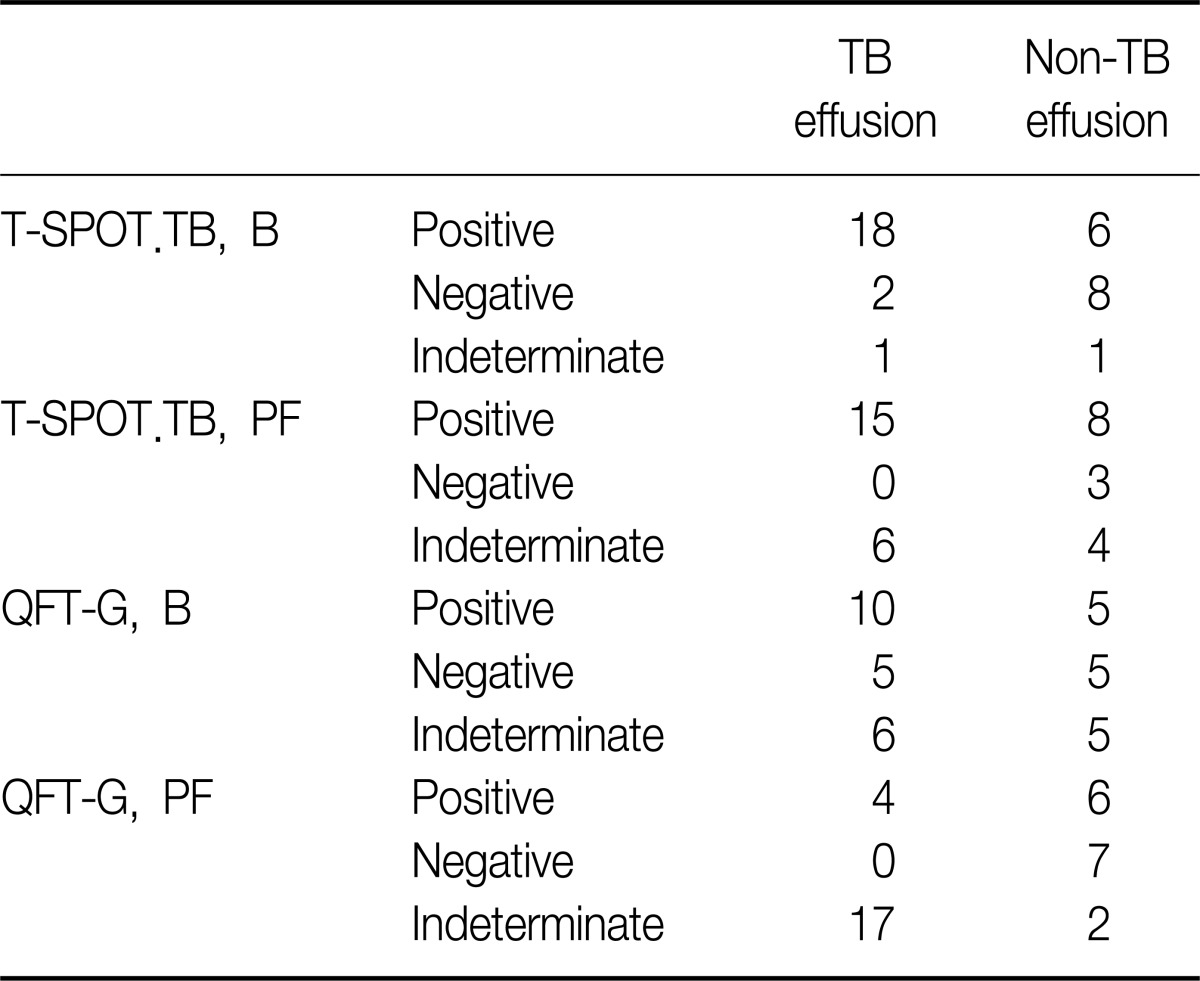
The sensitivity and specificity in blood were 85.7% and 53.3% for the T-SPOT.TB test and 47.6% and 33.3% for the QFT-G test, respectively. Applying the manufacturers' interpretation of results for blood to PF showed indeterminate results in 10 of 36 patients for the T-SPOT.TB test and in 19 of 36 patients for the QFT-G test, respectively (Table 2). The main cause of indeterrminate results in both IGRAs on PF was a high nil value in the tuberculous group.
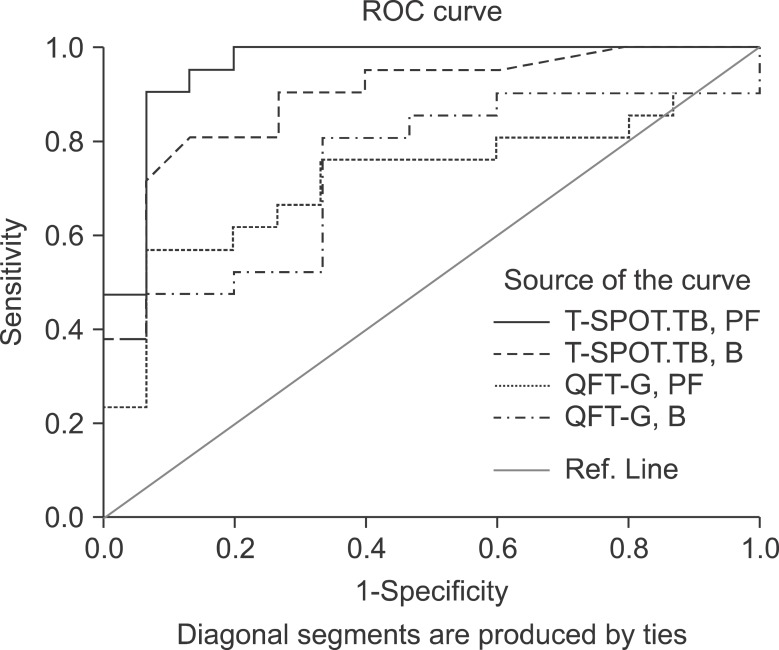
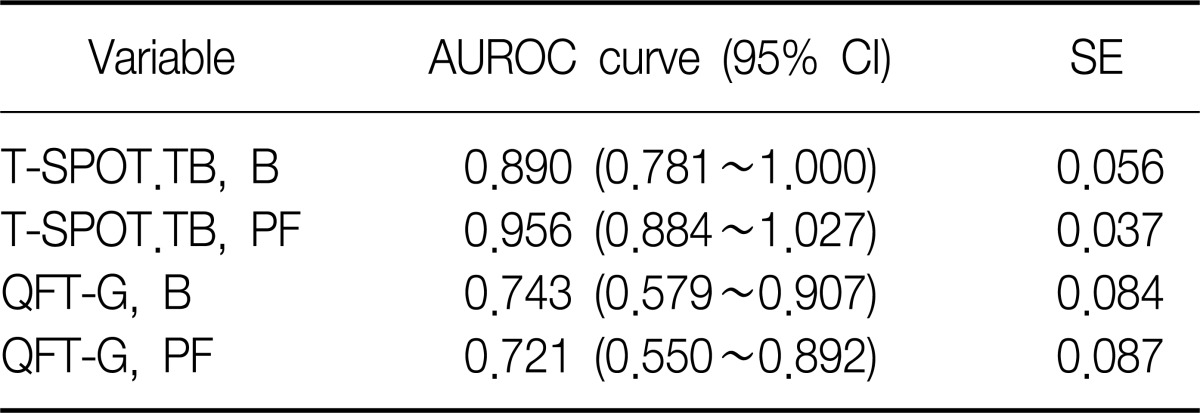
To evaluate the relative discriminative accuracy of the T-SPOT.TB and QFT-G assay in PF and blood, we assessed the ROC curve of each test. The ROC curve was the greatest for the T-SPOT.
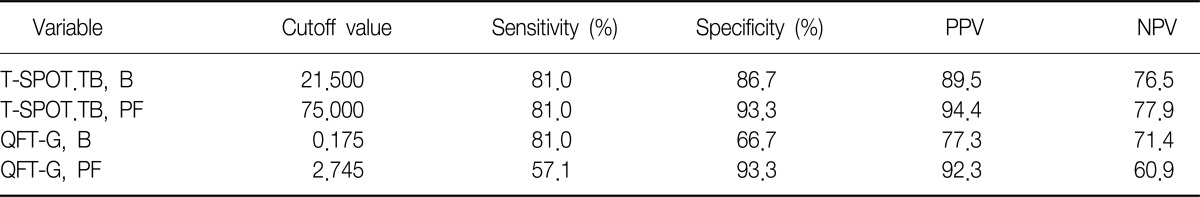
TB test in PF, followed by the T-SPOT.TB test in blood, QFT-G test in blood, and QFT-G test in PF (Figure 3). The respective area under the ROC curve were 0.956, 0.890, 0.743, and 0.721 (Table 3). We chose a cutoff value for each test that maximized the specificity without a significant loss of sensitivity. For the PF T-SPOT.TB test, a cutoff value of >75 spot counts improved the specificity (93.3%) with a minor decrease in sensitivity (90.5%), and showed a 94.4% positive predictive value and 77.8% negative predictive value. For the PF QFT-G test, a cutoff of IFN-╬│ level >2.745 IU/mL produced a sensitivity of 57.1%, specificity of 93.3%, positive predictive value of 92.3%, and negative predictive value of 60.9%. The best cutoff values of the two IGRAs were higher in PF than in blood (Table 4).
We prospectively investigated the clinical utility of the T-SPOT.TB and QFT-G tests performed on PF and blood samples for diagnosing tuberculous pleurisy in a head-to-head comparison. In this study, the T-SPOT.TB assay using PF had the greatest diagnostic accuracy for differentiating tuberculous pleurisy in non-HIV patients in a country with an intermediate incidence of TB infection. The T-SPOT.TB test also produced fewer indeterminate results than the QFT-G test and showed a significant change in the number of IFN-╬│ spot-forming cells between PF and blood within the tuberculous pleurisy group.
Comparing the diagnostic performance of either IGRA between PF and blood samples in the TB pleurisy, some clinical studies showed inconsistent results, depending on the type of assay, patient population, and incidence of TB infection12,15-20. In countries with a low TB burden, the IGRA has superior diagnostic accuracy in PF than in blood, whereas the reverse is true in intermediate-to high-burden countries19,20. In the current study, we showed that the T-SPOT.TB test had a higher diagnostic performance in PF, whereas the QFT-G test had poorer efficacy in PF. However, few studies have directly compared the performance of two IGRAs for active TB infection, especially for TB pleurisy. In 200 patients with suspected TB, Lai et al.21 reported that the T-SPOT.TB test had a higher sensitivity and produced fewer indeterminate results than the QFT-Gold in-tube (QFT-GIT) assay. To our knowledge, only one report, by Dheda et al.22, directly compared the T-SPOT.TB and QFT methods in PF for the diagnosis of the tuberculous pleurisy. Dheda et al.22 also showed that the PF T-SPOT.TB test had a higher ROC than the PF QFT-GIT test, a finding that is similar to ours. Whereas Dheda et al.22 included patients from a country with a high TB burden and half of whom were HIV positive, nearly all of our patients were immunecompetent patients and were studied in an intermediate TB burden setting. A recent meta-analysis23 analyzed the diagnostic accuracy of IGRAs for diagnosing active TB and showed that the T-SPOT.TB test using extrasanguineous fluids is currently the best immunodiagnostic method.
There are some reasons for the superiority of the T-SPOT.TB assay using PF among the IGRAs in our study. First, the T-SPOT.TB assay but not the QFT test requires a mandatory number of mononuclear cells, which might ensure a more accurate result even in patients with low T cell titers, such as those with HIV infection or another immunodeficiency. Second, more accurate results may be obtained when performing the IGRA in PF, the active infection site of tuberculous pleurisy, because of the compartmentalization of the immune response of Th1 cells in TB infection12,16-18,22. Third, in our study, the QFT-G test had more indeterminate interpretations than the T-SPOT.TB test in both PF and blood, which might reduce its diagnostic accuracy.
The findings about inconclusive results of the two IGRAs in the present study are consistent with the meta-analysis by Sester et al.23, who demonstrated that indeterminate results are common in the QFT test and more frequent in PF than in blood (23.1% and 7%, respectively). By contrast, the T-SPOT.TB test showed a similar frequency of indeterminate results between PF and blood (5% and 3.4%, respectively). The causes of indeterminate results in the ELISA method in our study were high nil value in the TB group and a weak response to the mitogen in the non-TB group. It is supposed that high IFN-╬│ response in the negative control could occur due to higher rate of inflammation, such as coexisting or transient infection15,24. In addition, the weak response to the positive control in the non-tuberculous group may reflect an unverified suppressed immune status. The nontuberculous group had older patients than the tuberculous group, and the older patients might have lower immune responses. Further large-scale research is needed to solve problems, such as the considerable number of indeterminate results and to identify the best cut-off values, for applying IGRAs to PF for diagnosing TB pleurisy.
The current study has several limitations. First, the number of cases was small, and some cases of active TB were diagnosed based on clinical grounds rather than microbiological confirmation. However, restricting the analysis to culture-confirmed TB cases did not change the results. Second, we used QFT-G assay rather than the new QFT-GIT assay, which includes another TB-specific antigen, TB 7.7. Although the QFT-GIT test might be presumed to have superior diagnostic accuracy compared with the QFT-G test, a systemic review by Pai et al.25 showed that the two QFT assays have similar sensitivity and specificity for the diagnosis of latent TB infection. In conclusion, the PF T-SPOT.TB test showed highest diagnostic accuracy among the IGRAs using blood and PF in the detection of tuberculous pleurisy in an intermediate-burden setting of TB infection. It suggests that T-SPOT.TB assay, especially applied directly to PF, may be an adjunctive, but useful method in the diagnosis of tuberculous pleurisy.
Acknowledgements
The statistical consultation was supported by Catholic Research Coordinating Center of the Korea Health 21 R&D Project (A070001), Ministry of Health & Welfare, Republic of Korea.
References
1. Korean Academy of Tuberculosis and Respiratory Disease. Guideline for diagnosis and management of tuberculosis. 2005. Seoul: Korean Academy of Tuberculosis and Respiratory Disease.
2. Seibert AF, Haynes J Jr, Middleton R, Bass JB Jr. Tuberculous pleural effusion: twenty-year experience. Chest 1991;99:883-886. PMID: 1901261.


3. Gopi A, Madhavan SM, Sharma SK, Sahn SA. Diagnosis and treatment of tuberculous pleural effusion in 2006. Chest 2007;131:880-889. PMID: 17356108.


4. Vald├®s L, Alvarez D, San Jos├® E, Penela P, Valle JM, Garc├Ła-Pazos JM, et al. Tuberculous pleurisy: a study of 254 patients. Arch Intern Med 1998;158:2017-2021. PMID: 9778201.


5. Burgess LJ, Maritz FJ, Le Roux I, Taljaard JJ. Combined use of pleural adenosine deaminase with lymphocyte/neutrophil ratio: increased specificity for the diagnosis of tuberculous pleuritis. Chest 1996;109:414-419. PMID: 8620715.


6. Lalvani A. Diagnosing tuberculosis infection in the 21st century: new tools to tackle an old enemy. Chest 2007;131:1898-1906. PMID: 17565023.


7. Pai M, Riley LW, Colford JM Jr. Interferon-gamma assays in the immunodiagnosis of tuberculosis: a systematic review. Lancet Infect Dis 2004;4:761-776. PMID: 15567126.


8. Pai M, Zwerling A, Menzies D. Systematic review: T-cell-based assays for the diagnosis of latent tuberculosis infection: an update. Ann Intern Med 2008;149:177-184. PMID: 18593687.



9. Barnes PF, Mistry SD, Cooper CL, Pirmez C, Rea TH, Modlin RL. Compartmentalization of a CD4XMLLink_XYZ T lymphocyte subpopulation in tuberculous pleuritis. J Immunol 1989;142:1114-1119. PMID: 2464638.

10. Nemeth J, Winkler HM, Zwick RH, Rumetshofer R, Schenk P, Burghuber OC, et al. Recruitment of Mycobacterium tuberculosis specific CD4XMLLink_XYZ T cells to the site of infection for diagnosis of active tuberculosis. J Intern Med 2009;265:163-168. PMID: 18793244.


11. Jafari C, Ernst M, Kalsdorf B, Greinert U, Diel R, Kirsten D, et al. Rapid diagnosis of smear-negative tuberculosis by bronchoalveolar lavage enzyme-linked immunospot. Am J Respir Crit Care Med 2006;174:1048-1054. PMID: 16858013.


12. Ates G, Yildiz T, Ortakoylu MG, Ozekinci T, Erturk B, Akyildiz L, et al. Adapted T cell interferon-gamma release assay for the diagnosis of pleural tuberculosis. Respiration 2011;82:351-357. PMID: 21293103.


13. Lee JY, Choi HJ, Park IN, Hong SB, Oh YM, Lim CM, et al. Comparison of two commercial interferon-gamma assays for diagnosing Mycobacterium tuberculosis infection. Eur Respir J 2006;28:24-30. PMID: 16611658.


14. Kang YA, Lee HW, Yoon HI, Cho B, Han SK, Shim YS, et al. Discrepancy between the tuberculin skin test and the whole-blood interferon gamma assay for the diagnosis of latent tuberculosis infection in an intermediate tuberculosis-burden country. JAMA 2005;293:2756-2761. PMID: 15941805.


15. Baba K, S├Ėrnes S, Hoosen AA, Lekabe JM, Mpe MJ, Langeland N, et al. Evaluation of immune responses in HIV infected patients with pleural tuberculosis by the QuantiFERON TB-Gold interferon-gamma assay. BMC Infect Dis 2008;8:35PMID: 18366633.




16. Losi M, Bossink A, Codecasa L, Jafari C, Ernst M, Thijsen S, et al. Use of a T-cell interferon-gamma release assay for the diagnosis of tuberculous pleurisy. Eur Respir J 2007;30:1173-1179. PMID: 17715165.


17. Chegou NN, Walzl G, Bolliger CT, Diacon AH, van den Heuvel MM. Evaluation of adapted whole-blood interferon-gamma release assays for the diagnosis of pleural tuberculosis. Respiration 2008;76:131-138. PMID: 18434705.


18. Lee LN, Chou CH, Wang JY, Hsu HL, Tsai TH, Jan IS, et al. Enzyme-linked immunospot assay for interferon-gamma in the diagnosis of tuberculous pleurisy. Clin Microbiol Infect 2009;15:173-179. PMID: 19154487.

19. Joshi R, Pai M. Can pleural tuberculosis be diagnosed using interferon-gamma release assays? Respiration 2008;76:128-130. PMID: 18708735.


20. Hooper CE, Lee YC, Maskell NA. Interferon-gamma release assays for the diagnosis of TB pleural effusions: hype or real hope? Curr Opin Pulm Med 2009;15:358-365. PMID: 19417671.


21. Lai CC, Tan CK, Lin SH, Liao CH, Huang YT, Hsueh PR. Diagnostic performance of whole-blood interferon-gamma assay and enzyme-linked immunospot assay for active tuberculosis'. Diagn Microbiol Infect Dis 2011;71:139-143. PMID: 21840675.


22. Dheda K, van Zyl-Smit RN, Sechi LA, Badri M, Meldau R, Meldau S, et al. Utility of quantitative T-cell responses versus unstimulated interferon-(gamma) for the diagnosis of pleural tuberculosis. Eur Respir J 2009;34:1118-1126. PMID: 19386693.


23. Sester M, Sotgiu G, Lange C, Giehl C, Girardi E, Migliori GB, et al. Interferon-gamma release assays for the diagnosis of active tuberculosis: a systematic review and meta-analysis. Eur Respir J 2011;37:100-111. PMID: 20847080.


24. Trajman A, Pai M, Dheda K, van Zyl Smit R, Zwerling AA, Joshi R, et al. Novel tests for diagnosing tuberculous pleural effusion: what works and what does not? Eur Respir J 2008;31:1098-1106. PMID: 18448504.


25. Pai M, Zwerling A, Menzies D. Systematic review: T-cell-based assays for the diagnosis of latent tuberculosis infection: an update. Ann Intern Med 2008;149:177-184. PMID: 18593687.



Figure┬Ā1
Comparison of the numbers of interferon-gamma producing spot-forming cells (SFCs) using the T-SPOT.TB method in pleural fluid and in blood, between the pleural tuberculosis (plTB) and non-pleural TB (non-TB) groups. All results have been calculated after subtraction of SFC counts in the negative control wells. For group comparison by a Mann-Whitney test. NS: not significant. *p<0.005. ŌĆĀp<0.001.
Figure┬Ā2
The concentrations of interferon-gamma (IFN-╬│) using the QuantiFERON-TB Gold method in pleural fluid and in blood, between the pleural tuberculosis (plTB) and non-pleural TB (non-TB) groups. IFN-╬│ values have been subtracted from the corresponding background control values. For group comparison by Mann-Whitney test. NS: not significant. *p<0.05. ŌĆĀp<0.01.
Figure┬Ā3
Receiver operating characteristic curves between T-SPOT.TB and QuantiFERON-TB Gold (QFT-G) test for the diagnosis of tuberculous pleurisy. ROC: receiver operating characteristic; PF: pleural fluid; B: peripheral blood.
Table┬Ā1
Clinical characteristics of the patients
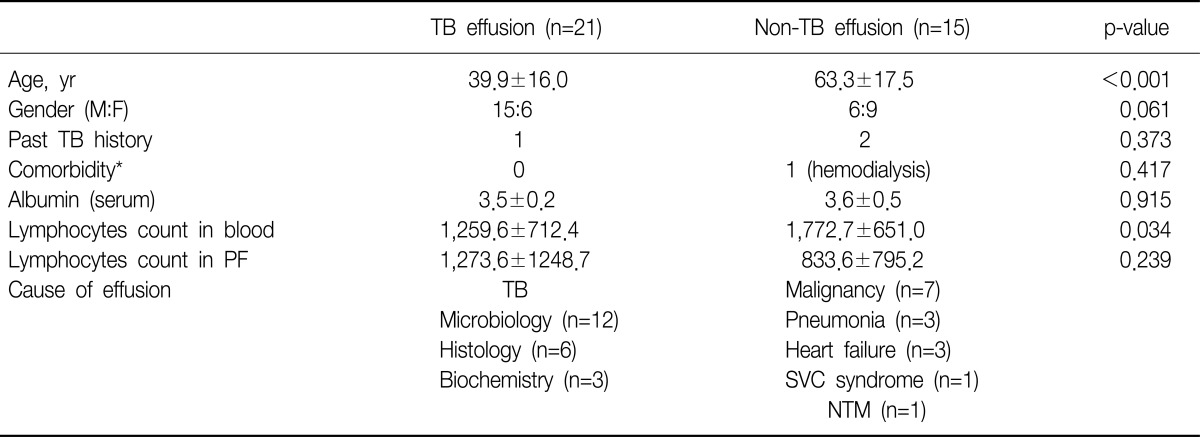
*Diseases requiring immunosuppressive drugs, undergoing hemodialysis, hematologic malignancy, diabetes mellitus, or HIV infection.
TB: tuberculosis; M: male; F: female; Blood: peripheral blood; PF: pleural fluid; SVC syndrome: superior vena cava syndrome; NTM: nontuberculous mycobacterium; HIV: human immunodeficiency virus.
Table┬Ā2
Interpretation of two interferon-gamma release assays in pleural fluid and in blood, between the tuberculous and nontuberculous effusion group


 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Print
Print Download Citation
Download Citation




